
DJC.COM
April 23, 2009
New air system could keep patients warmer and healthier
CDi Engineers

Connell
|
What’s expensive, resource-hungry and really cold? Okay, besides a top-of-the-line snowmobile. It’s that blast of freezing air that shoots down from the ceiling providing a change of room air every 10 minutes in a hospital patient room.
But recent research confirms that there’s a better way to ventilate health care facilities — with kinder, gentler and warmer air flowing up from the floor level. Called displacement ventilation, this technology reduces air changes per hour, chilled water requirements, simultaneous heating and cooling, and related costs — and creates a cozy, inviting and safe breathing environment.
Air from below
Traditional hospital ventilation systems introduce air from near the ceiling, force it downwards with a diffuser, and then suck it back out through an exhaust grille, also at ceiling level.
This intentionally causes a swirling effect to improve average room temperatures but it also entrains contaminants along with the air and thus circulates germs. It also creates that North Pole feeling due to the high air exchange rates presently required by code for health care facilities.
Displacement ventilation, on the other hand, introduces slightly warmer air at a lower velocity through vents near the floor on side walls. The air pools across the floor, picks up heat from the room, occupant or heat-generating equipment, and rises up through to the breathing zone, where most contaminants are found.
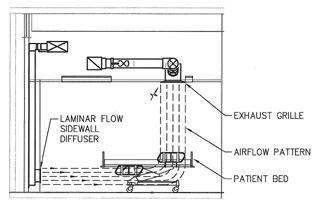
Image by CDi Engineers In a displacement ventilation system, warmer air enters through vents near the floor, then rises and exits through exhausts in the ceiling, carrying out contaminants without mixing them into the room air. |
The goal is to provide temperature conditioning only in the occupied volume of the room, not the upper empty reaches, and carry contaminants directly out of the occupied zone without mixing them into the room air. The system is not only more comfortable for occupants, but effectively protects both staff and patients from germs.
Economies are significant. Displacement ventilation requires only four air changes per hour, a reduction of one third over traditional methods. Less air at a higher temperature translates into less energy required to chill and deliver the air. Engineers estimate that total energy ventilation cost reductions can be as high as 30 percent.
Lower energy costs
While displacement ventilation is well accepted in commercial settings, health care facilities have lagged behind in the use of such systems for patients.
This is understandable because clean, properly circulating air is so vital to patient recovery and comfort, and hospitals tend to be very conservative. But hospitals also operate around the clock, every day of the week, creating very high energy costs, and are therefore now investigating solutions that can save money without negatively impacting patients and health care providers.
Change is in the air. Just two months ago, the health-management organization Kaiser Permanente cut the ribbon on North America’s first displacement ventilation system at its acute care facility in Modesto, Calif.
Kaiser installed displacement ventilation systems in the facility’s inpatient rooms and the emergency room as part of a research study to compare overhead, displacement and natural ventilation. Inpatient rooms represent a significant portion of hospital space, and the emergency room is one of the areas of highest concern for airborne infection transmission from undiagnosed contagious patients.
Initial findings indicate that Kaiser will reduce the energy costs of ventilation by as much as 30 percent with the new ventilation approach, while still maintaining infection control. More detailed results will be released later this year.
Air quality
Academics have been interested in health care applications for displacement ventilation, too.
Qingyan Chen of Purdue University conducted a comparative study on displacement and mixing (or traditional overhead) ventilation in a patient ward, and presented his findings at this year’s American Society of Healthcare Engineers (ASHE) annual Healthcare Planning, Design & Construction conference.
His goals were to determine whether displacement or mixing ventilation is superior for patient air quality, whether exhaust levels in the restroom impact air quality by source type, and whether coughing and breathing have different impacts on indoor air quality.
Chen found that displacement ventilation provides a low contaminant concentration in the lower parts of the room, and that high exhaust above the patient and through the restroom was very important for displacement ventilation, but not for mixed ventilation.
As might be expected, he found higher concentrations of contaminants at high locations with coughing cases compared with breathing cases. He also concluded that displacement ventilation with four air changes per hour can provide the same, if not better, air quality than mixing ventilation, provided that the exhausts are properly located.
His colleague, Weiran Xu of Mentor Graphics in Massachusetts, agreed. Conducting numerical analysis for the same study, Xu reported to the ASHE conference that the displacement ventilation system actually provided cleaner conditions at lower room levels, including the breathing zone, primarily due to air mixing occurring at lower areas in the room.
More like home
Displacement ventilation contributes to two growing tendencies in health care design: sustainability and a less institutional ambiance. Reducing air flow requirements both minimizes resource consumption and increases occupant comfort.
Technology also helps reduce the institutional feeling of a patient room. Designers are increasingly incorporating features that make a patient’s room seem more like home, minimizing stress and encouraging more frequent and longer visits from friends and family members. This carefully created atmosphere is nurtured with the help of a calmer, less-intrusive ventilation system.
Because displacement ventilation has so many benefits — cost savings, environmental friendliness and enhanced patient comfort — we can expect to see Puget Sound hospitals adopting Kaiser’s lead in the near future.
Jill Connell is an associate with CDi Engineers in Lynnwood.
Other Stories:
- Rural hospitals can build wisely if they have a plan
- New health care construction: Always costly, rarely needed
- When electronic systems 'talk,' patients, hospitals benefit
- Hospital project prices falling, but it is still buyer beware
- Architects: Listen and learn from your clients
- Designing to get the most bang for your buck
- Lean design cuts cost for Covington medical building
Copyright ©2009 Seattle Daily Journal and DJC.COM.
Comments? Questions? Contact us.