
DJC.COM
November 16, 2006
State to adopt national health care design standards
CDi Engineers

Moeller
|
For decades, Washington’s health care design codes were similar (but not identical) to national standards maintained by the Facility Guidelines Institute and published by the American Institute of Architects.
As a result, Washington is one of only eight states that did not opt into the national protocols for new hospital construction, which were formed several decades ago and now come under the administration of the FGI.
That changes in mid-2007, when Washington intends to hop aboard and adopt the AIA/FGI guidelines as standards.
The move means that we finally align with standards that are continually reviewed and updated, and are supported by a nationwide network of professionals involved in all aspects of health care design, construction, management and maintenance.
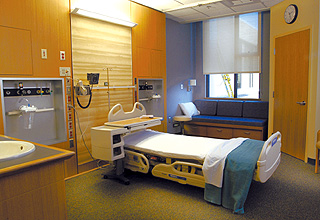
Photo courtesy of CDi Engineers New hospital design guidelines call for 120 square feet of clear floor area per patient room, an increase of 20 square feet. The change is to make room for bulky medical equipment such as carts and stands. |
It also points to some big modifications in the way hospitals and other facilities will be designed in the future, impacting almost anyone involved in the health care building industry.
1 patient per room
Concerned about you or a family member being stuck with a noisy roommate in the hospital? What if you checked into a hotel, and they tell you that you’re going to be sharing a room with a complete stranger? In hospitals this happens all of the time, and you have little or no say about it.
The guidelines require that new hospitals will have only one patient per room, unless the necessity of a two-bed arrangement can be demonstrated. In addition, if an older facility is being renovated, it cannot increase the current capacity of each room or exceed a maximum of four patients.
This will greatly reduce the number of patients a hospital can accommodate per square foot. However, it will also reduce the chances of cross-infection from one patient to another and increase the privacy of the patient environment, one of the main goals of the guidelines.
While Washington’s existing code allows four patients to a room, most newer hospitals are already going to single-room layouts. Some rural or smaller hospitals, however, may not be able to easily afford private rooms. They will be able to petition the licensing authority for a waiver.
More space
| Design guidelines |
|
The 2006 edition of the AIA/FGI Guidelines for Design and Construction of Health Care Facilities may be purchased online at http://www.fgiguidelines.org.
|
Similarly, the new guidelines call for 120 square feet of clear floor area per patient room, compared with the 100 feet currently mandated by Washington state.
One of the drivers of the increased space is the recognition that patient rooms are becoming cluttered with equipment, some of which is on a cart or stand with a large footprint. The stricter ruling will help make the rooms safer and easier for health care professionals to work in.
In critical care units, the current code calls for a minimum of 150 square feet per patient. The new minimum is 200 square feet, a significant allowance for increased technology around the patient.
New ventilation rules
A change that impacts mechanical engineers is the requirement that all return ventilation serving patient areas must be ducted. Exceptions are areas used for administrative, dining, lobby, engineering, housekeeping and maintenance purposes.
Also, the new guidelines prohibit reversible airflows from being used in infection isolation rooms. The current code in Washington did not address this issue, opening the possibility for infections to spread through the hospital.
A requirement has been added for renovations that states if system modifications affect greater than 10 percent of the system capacity, designers shall utilize pre-renovation water/air flow measurements to verify that sufficient capacity is available and that renovations have not adversely affected flow rates in non-renovated areas.
The new guidelines also reflect a growing alliance with other professional organizations such as the American Society of Heating, Refrigerating and Air-Conditioning Engineers by recognizing their position and efforts to provide guidance for mechanical systems in health care.
Broad reach
The new codes apply to more than just hospitals, however. Chapters in the guidelines dealing with hospice, assisted living and adult day health care have been greatly expanded. In addition, a brand-new chapter speaks to the needs of small primary-care hospitals.
When it comes to renovation, the jury is still out on what effect the guidelines will have. There are more provisions in the guidelines that allow more leeway in renovations than is currently included in state codes. For years, any construction was considered new construction by the state and enforced as such.
The guidelines address the renovation issue by making allowances for existing space requirements to remain at past levels of compliance.
Defining renovation as opposed to new construction can be an emotional and costly subject. The renovation requirements can sometimes make the difference between moving forward with a much-needed change or canceling the project for economic reasons.
More flexibility
What the new guidelines do, in effect, is to set the minimum bar using evidence-based data. More important, it allows the facility to determine how it is going to deliver patient care, and operate its business through its functional program — it gives more flexibility than the current codes. Many in the state are already looking to the future and implementing the guidelines as part of their goal to provide national-level care.
We now have access to industry-leading professionals, many of whom have been working on the guidelines since their inception decades ago. They understand both the spirit and letter of the codes and have no axe to grind. They can therefore provide us with high-level support that wasn’t previously available to Washington design professionals and the Department of Health under the old process.
A second benefit comes from the quality of the Health Guidelines Revision Committee itself. Its 125 members include some of the best-known physicians, architects, engineers, facilities experts, health care administrators, authorities having jurisdiction and infectious control professionals in the country.
They bring a phenomenal background of knowledge and health care experience to the table, including access to a multitude of evidence-based research ensuring that the industry is being guided in the right direction.
These benefits explain why the Washington State Society for Healthcare Engineering has also been so involved in adoption of the guidelines. This group of health care professionals has been proactive in adding their knowledge and experience to Washington’s adoption process. It helps that every state is able to write its own amendments to the guidelines, too.
As a group, the society has proposed several amendments that make a lot of sense for our state, such as the ability to challenge the single-bed requirement, humidification and decontamination issues and other pertinent items.
Richard Moeller is president of CDi Engineers, a mechanical engineering firm in Lynnwood. He also serves on the Health Guidelines Revision Committee of the Facilities Guidelines Institute.
Other Stories:
- Hospital gardens help patients heal
- New law encourages hospitals to give patients a lift
- Hotels offer lessons for Oregon hospital
- Quick! Turn an office building into a medical center
- Complex projects call for virtual construction
- Build a better building with 3-D modeling
- Boomers shaping future of health care design
Copyright ©2009 Seattle Daily Journal and DJC.COM.
Comments? Questions? Contact us.