|
Subscribe / Renew |
|
|
Contact Us |
|
| ► Subscribe to our Free Weekly Newsletter | |
| home | Welcome, sign in or click here to subscribe. | login |
Construction
| |
 |
August 27, 2020
Modified mechanical systems for healthier schools
BCE Engineers

Caffee
|
In the current climate, it’s no secret that the transmission of respiratory illnesses has become a primary concern in every facet of life. School districts, bound by a finite academic year compounded by grade-level standards, are chief among those grappling with how to safely reopen.
The good news is that mechanical systems in new schools are already being designed using proven techniques to combat the threat of airborne transmission. Best practices like utilizing outside air ventilation and not recirculating air while the building is occupied are key factors employed on every project to keep the air within the building fresh and clean.
But will this make a difference when schools reopen? What about older schools that haven’t been updated in decades?
While we are not virus dispersion experts, using information known at this time about the spread of viruses, and in particular COVID-19, we can make recommendations to help reduce transmission possibilities.
In general, the job of the HVAC system is to fully mix the air in a room to provide an even comfort level for the occupants. Unfortunately, while mixing the air, airborne and near airborne viruses are also mixed within the room. This means a good HVAC system is also a good viral transmitter. COVID-19, in particular, seems to be locally transmitted. This means that it is less likely to get into the ductwork than true airborne viruses, but is more effectively spread within the space that the infected person is located. Fortunately, there are measures that can be taken to minimize the transmission potential.
Whether a school has a new HVAC system or is looking to retrofit an existing system, the following ideas may help reduce the spread of viruses and can lead to healthier schools. Of course, there are many different HVAC systems in which to apply different technologies and all of those systems will have individual idiosyncrasies that will need to be addressed with each option.
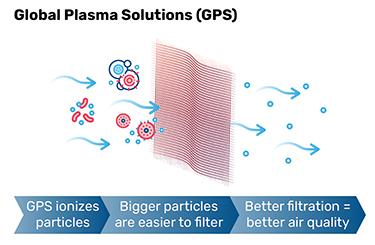
• Global Plasma Solutions: Global Plasma Solutions (GPS) can be added to the return air stream of a recirculating HVAC unit. GPS ionizes particles to cause them to stick to each other. This makes bigger particles that are easier to filter. Better filtration leads to better air quality. While the particles are collecting together, viruses may also be bound to the particle clusters and filter out of the airstream with greater effectiveness. GPS systems can easily be retrofitted into existing equipment, as well as new design.
• Powered filters: Powered filters can be added to ducted HVAC systems. Powered filters operate by statically charging filter media to attract particles and have the ability to filter better at lower pressure drops. Powered filters work well with the GPS systems to better filter the air while reducing filter maintenance. They are convenient for retrofits and new designs.
• Humidification: Keeping humidification between 40% and 60% relative humidity (RH) allows the human body to have optimum resistance for airborne and semi-airborne viruses. In the Northwest, the indoor RH is normally in this range except in the wintertime. In the winter, humidity indoors typically drops to around 25% RH. At that level of humidity, viruses penetrate the lung tissue more deeply and increase the potential infection and severity of the infection. Humidity levels work for traditional viruses. However, it is not clear if it works for COVID-19 because currently that virus is quite active in the summer in the southern U.S. where the humidity is high. Humidification is relatively easy to retrofit on existing central systems and very difficult to retrofit on decentralized systems.
• Increasing outside airflow: Increasing outside airflow dilutes viruses in the air and reduces the potential for infection by a large concentration of virus. However, there are many constraints on just increasing outside airflow. Systems with economizers can easily increase the outside air during mild days (not the coldest or hottest design days) without sacrificing room comfort. Systems without economizers will need to have their capacity checked to see if they are capable of adding extra ventilation quantities. However, in both cases, energy use will increase and thus operational costs.
• Effective ventilation: Effective ventilation is supplying high and returning low or supplying low and returning high. There is still a complete mixing of the air, but the ventilation quantities are more effective. This can allow for lower outside air quantities to comply with code or allows for code maximum quantities to better dilute room contaminates. Effective ventilation can be used to reduce the density of the virus within the room. Effective ventilation is difficult to add to an existing system, but is easy to design into a new system.
• Displacement ventilation: Displacement ventilation is supplying ventilation air low at laminar airflow speeds and slowly lifting the air to high returns. The difference between displacement ventilation and effective ventilation is that effective ventilation is still meant to fully mix the air in the room and displacement ventilation is meant just to treat the breathing zone. Displacement ventilation allows the air around the person to lift directly upwards and attempts to not mix the room. This will limit the spread of contaminates and viruses to just around a particular infected person. Displacement systems cannot be retrofitted into existing systems.
• Ultraviolet treatment: UV light is an effective virus sanitizer. It takes very little time for direct UV light to destroy a virus. UV lights can be put into the supply air stream (after heat exchangers and coils) to destroy viruses. UV lights are best with recirculating systems and less effective with 100% outside air systems. They work best in new design.
• Electric hand dryers: Electric hand driers use recirculated, heated bathroom air to dry previously washed hands. Since the air does not get hot enough to sanitize the virus, this is a potential spot for reinfection. Touchless paper towel dispensers can be a safer alternative.
Chris Caffee is a principal and mechanical engineer at BCE Engineers.
Other Stories:
- Building schools is about building communities
- Learning inside and outside the box
- First U.S. net zero school has 10-year checkup
- How the pandemic can change education for the better
- Eastside school’s HVAC system zaps the bad stuff
- Idaho school master plan takes on Living Building Challenge
- Community engagement drives design for Tacoma school
- Modular classrooms are a quick study in filling vital needs
- Students get a boost from outdoor connections
- UWT project focuses on equity, justice and design