|
Subscribe / Renew |
|
|
Contact Us |
|
| ► Subscribe to our Free Weekly Newsletter | |
| home | Welcome, sign in or click here to subscribe. | login |
Construction
| |
 |
June 23, 2011
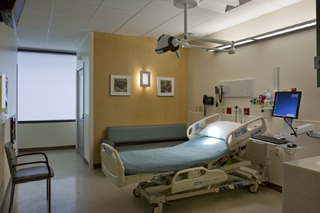
‘Hybrid’ rooms a low-cost answer to space needs
Sparling

Ramundo
|
Over the past few decades health care has become more complex and specialized. Hospitals have responded by developing distinctly different physical patient spaces for each specialty. However, many of these specialized spaces are underutilized due to the small number of appropriate patients for the particular room type.
Given the current dedication of so many resources to specialty care it is not unusual to have empty beds yet at the same time have patients waiting for a particular type of dedicated bed that is not available.
As health care organizations build new facilities, they must consider the emerging industry trends and develop creative spaces that will provide functional flexibility over the years. As baby boomers get older they will become more frequent consumers of health care, resulting in increasing numbers of emergency room visits and admissions to inpatient care.
Also, more and more, surgical patients are going home the same day and do not have an inpatient bed to go to, and so they must fully recover in the post-anesthesia care unit, sometimes causing a backup in these beds. These dynamics are placing an escalating demand on hospitals to maximize the capacity of their patient care resources and to create flexible solutions without increasing costs.
Soon, with changes in Medicare and commercial insurance reimbursements, only the sickest patients will be admitted to inpatient units in the hospital.
If a patient’s condition worsens, he or she would typically be transferred to a specialized intensive care unit (ICU) bed. In addition to concerns about availability of the specialized ICU bed and the wait time for the room to be ready, there are inherent risks in transferring a patient from one unit to another.
Studies have demonstrated that moving a patient between departments increases the risk for errors and infection. These transfers are stressful and costly, using staff time to prepare the patient, family and medical records and the physical transportation to the ICU.
Another option is the use of hybrid rooms, which are outfitted to bring ICU equipment to the patient rather than move the patient to another unit. The specialized care is then provided in the original general-purpose room.
With changes in patient demographics, reimbursement and technology, the health care industry is seeing new norms evolve:
• Reimbursement models have caused more care to be delivered on an outpatient basis, leaving only the sickest patients in the hospital.
• Private rooms are increasingly seen to provide a better healing environment, more privacy and fewer hospital-acquired infections.
• Patient care units may be repurposed to provide resources for a different type of care than originally intended.
A flexible format
Organizations are seeking ways to achieve flexibility for future needs. A space with a narrowly specified use may be difficult to use for another purpose in eight years.
There have been major advancements in health care technology and its integration into patient care. There will continue to be new technologies coming on to the health care scene, and hospitals must be able to incorporate these.
The high cost of construction is causing hospital administrators to seek building solutions that will not become obsolete and require reinvestment within a decade of opening. Thus the concept emerged of a flexible patient room design that could accommodate a variety of patient types, an increasingly higher-acuity mix of patients, and new technologies over its extended life. These rooms are often referred to as “hybrid” rooms, “universal care” rooms or “acuity adaptable” rooms.
Hybrid rooms have both short- and long-term advantages. Clearly it is simpler and less expensive in the long run to build in flexibility during a renovation or a new build. Retrofitting older patient rooms is costly and inconvenient.
In the short term, a patient room can be equipped with sufficient medical gases, electric outlets, suction, supply storage, and physiologic monitor rack- and network-connectivity to allow the following uses:
• Move ICU equipment into the room to provide higher acuity care without moving the patient to another unit.
• Bring in telehealth equipment for medical consultations and monitoring.
• Vary the type of patients that can be accommodated across the day, such as pre-op patients being checked in during the morning, recovering post-op patients in the afternoon, and emergency room overflow during peak evening hours.
Equipping a room for long-term adaptability requires:
• Additional network drops to accommodate future technologies.
• Consideration of clearances and tolerances for obese patients.
• Building more than the minimum of laminar flow and isolation rooms.
• Ubiquitous computing to allow fully digital electronic medical records, including fixed stations and mobile devices.
Pros and cons
Historically, the concept of a hybrid space has worked well for obstetrics with the development of labor, delivery and recovery rooms, providing a flexible space that supports all levels of care needed in the birthing process.
Patients remain in one room, and as their needs change through the birth, the room is adapted to provide the needed resources. The patient does not have to move from room to room, yet is still provided the same care in this single, flexible room.
Operating rooms are beginning to establish hybrid operating rooms to accommodate the surgical patient whose procedure may start out as a closed, minimally invasive surgery and changes mid-procedure to an open surgery.
The flexibility of the room allows for the change in procedure without moving the anesthetized patient with open surgical sites down the hall to another room. This approach decreases the risks for prolonged anesthesia, infection and possible injury due to the physical move.
These successful uses of hybrid patient care space can encourage the further development of hybrid patient rooms, which can accommodate different sorts of patients and procedures. While some organizations have experienced great success with hybrid patient rooms, others have not found the concept to produce the results they were seeking.
Realized benefits:
• Improved patient satisfaction.
• Decreased patient safety incidents.
• Improved admission wait times.
• Increased staff satisfaction.
Challenges:
• Maintaining appropriate staff education.
• Additional cost of equipping rooms for flexibility.
• Increased staff turnover.
While the results of installing hybrid patient units are mixed, the health care industry faces significant challenges and must be open to considering new solutions. It is possible to learn from others’ results, and utilize the effective concepts for developing a customized solution.
When developing a new facility and considering the use of hybrid rooms, it would be advantageous to pilot the concept in an existing facility before building new dedicated resources. Develop and operate a hybrid patient unit with existing staff and conduct regular, frequent evaluations of the performance.
Assess the effectiveness of the hybrid room with a variety of scenarios: Is the flexible room effective with a patient whose condition worsens and requires an intensive-care level of treatment? Can the hybrid room successfully provide the needed environment for a variety of patient types in a given day, such as pre-op and post-op patients, and emergency department fast-track and overflow patients? Do the benefits of the flexible room offset the additional equipment costs needed to outfit a patient room to accommodate multiple types of care?
We must keep on evaluating the effect of flexible-purpose rooms and share the results with our colleagues so we may continue to develop and improve this concept.
Debby Ramundo is a technology consultant for IT architecture at Sparling, a Seattle-based technology consulting firm that specializes in health care planning and design. Ramundo is a registered nurse.
Other Stories:
- 13 tips for choosing your medical space
- Study will help UW’s Montlake Tower cut energy costs
- Swedish Issaquah aligns design with patient needs
- Good signage points the way to better health care
- 'Novel' process lets Swedish Issaquah hit fast forward
- Swedish women’s cancer center a one-stop shop
- Group Health is designing its clinic of the future
- Puyallup hospital tower puts focus on patients
- Evergreen opens center closer to its patients
- New VA complex to treat ‘emerging’ war injuries
- Friday Harbor hospital aims to be nation’s greenest
- UW expansion stays on track despite big change in plans