|
Subscribe / Renew |
|
|
Contact Us |
|
| ► Subscribe to our Free Weekly Newsletter | |
| home | Welcome, sign in or click here to subscribe. | login |
Architecture & Engineering
| |
 |
June 24, 2010
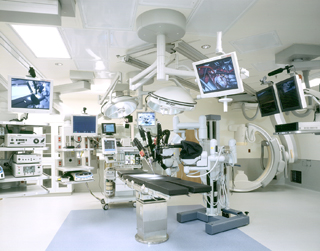
Surgical advances create ‘hybrid’ operating rooms
ZGF Architects
As new medical technologies enable a less-invasive approach to cardiac and vascular surgery, surgical specialists, radiologists and cardiologists are performing both diagnostic and therapeutic procedures in a sterile operating environment.
This shift in practice is blurring the boundaries between traditionally separate departments, staff, procedures, equipment and recovery spaces. As a result, operating room design continues to evolve to support these new procedures and technologies.
Hybrid operating rooms are emerging as a new and effective way to integrate advanced imaging technologies in surgical environments to increase efficiencies and utilization of resources while improving patient safety, experience and outcomes.
Why go hybrid?
Many surgical procedures benefit from the use of advanced imaging modalities, and many imaging studies now integrate surgery-type therapeutic interventions, especially in cardiac and vascular specialties. Research has shown clear benefits from designing adaptable environments that integrate these surgery and imaging services resulting in reduced morbidity (1.2 percent vs. 4.8 percent), hospital length of stay (3.4 days vs. 9.1 days) and recovery time (30 days vs. several months).
Hybrid rooms also facilitate multispecialty clinical collaboration resulting in imaging and technological advancements and superior medical training as surgeons become dual trained for both open and endovascular or catheter-insertion techniques. New procedures such as percutaneous heart valve replacements now undergoing clinical trials and testing in the United States will reduce the need for open heart surgery while increasing the demand for hybrid rooms.
Planning challenges
Combining both imaging and surgery capabilities in one hybrid room allows for real-time imaging during complex vascular or cardiac surgical procedures, yet presents many planning challenges ranging from integrating traditionally separate disciplines to determining the functional layout of the room to accommodate equipment and staff flow.
The major pieces of equipment that impact hybrid room layout include a surgical table, imaging equipment, lights and equipment booms. Coordination of these functional requirements involves resolving the spatial relationship between the equipment and staff flow needed for both open and closed procedures.
A digital operating suite completed in 2004 in Providence St. Vincent Medical Center’s facility in Portland functions as a hybrid room. As one of the first projects of its kind in the Northwest, the design team faced the additional challenge of planning the room while the medical equipment was still in development. This required the design to be as flexible as possible to support evolving technologies and procedures while meeting the needs of surgeons, radiologists and cardiologists.
Design of hybrid rooms requires technical coordination of the equipment with the existing building infrastructure. At Harborview Medical Center in Seattle, the only Level 1 trauma center serving Washington, Idaho, Montana, Wyoming and Alaska, a new hybrid room is being planned within the existing surgery suite to serve a large population of trauma and vascular patients.
Technical coordination of the room is complicated by the constraints of the existing mechanical systems, low floor-to-floor heights and spacing of the column grid. The design process is addressing workflow for surgery and imaging procedures with corresponding equipment needs and surgeon preferences.
Tools for problem solving
Solving the planning and technical coordination issues posed by the complex nature of hybrid rooms involves numerous face-to-face meetings with clinicians, architects, consulting engineers, contractors and equipment vendors, as well as site visits to recently completed hybrid rooms at other hospitals to “kick the tires.”
During the planning for the 28-room, two-level integrated surgical-interventional suite as part of new 350-bed hospital tower under construction for Providence Regional Medical Center Everett, the design team used 3-D modeling, enlarged color-coded floor plans, and a semi-transparent model using stacked plexiglass floor plates laminated with color floor plans to illustrate the dimensional relationships between services and routes for patients, staff and material transport. These tools helped facilitate discussion between diverse groups of clinicians and resolve operational challenges.
Currently in design, the phased expansion and remodel of a main operating suite at Providence Alaska Medical Center in Anchorage includes replacement of two cardiac operating rooms. Both are designed as hybrid rooms to serve cardiac surgery and other specialties as the technology develops.
Using a variety of tools, multidisciplinary workshops allowed clinicians to experiment with various room configurations. Full-scale room mock-ups of the favored room configurations allowed clinicians to simulate routine and emergency procedures as they evaluated equipment placement and the flow of patients, caregivers, supplies and information.
A role model
This new integrated model of care requires significant changes in existing operational practices and organizational culture that is not possible without the vision and leadership of dedicated clients, executive teams, key physicians and department heads.
It is our hope that successfully pioneering an approach to providing these integrated services will set a precedent for designing hybrid rooms now and in the future.
Jim Harman, Rosemary Carraher and Solvei Neiger are health care architects at ZGF Architects, and Barbara Anderson is a nurse medical planner at ZGF.
Other Stories:
- Mental health clinic breaking ground in Burien
- Hospitals: get ready for climate change laws
- Federal program keeps money flowing for hospital projects
- MultiCare opens $117M Tacoma campus expansion
- Robots bring changes to operating room design
- In wake of reform, hospitals try doing more with less
- Hospital noise rules get an update