|
Subscribe / Renew |
|
|
Contact Us |
|
| ► Subscribe to our Free Weekly Newsletter | |
| home | Welcome, sign in or click here to subscribe. | login |
Architecture & Engineering
| |
 |
June 24, 2010
Robots bring changes to operating room design
Mahlum

Goodfriend
|
The shift toward less-invasive surgery is creating significant changes in the design of surgical suites.
Driven by increased competition for outpatient volumes, greater volumes of high-acuity inpatient cases and a drive toward minimally invasive techniques, hospitals are changing how they use operating rooms as they add sophisticated new equipment and technology.
Three kinds of operating rooms are leading the way:
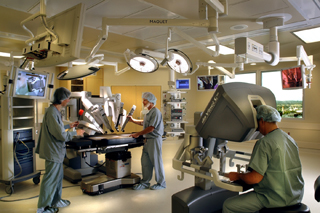
• Robotic. The most dramatic of the three, robotic surgical systems such as the da Vinci system employ a series of arms that have “fingers” equipped with cameras, lights, scalpels and suturing devices — all operated by a surgeon at a remote console. Cases have been carried out by surgeons located at devices remote from the hospital or even across the country.
More than 1,000 such systems have been installed thus far in the United States, including Swedish Medical Center in Seattle and Providence Sacred Heart Medical Center in Spokane. Initially the case load was focused on cardiac cases, but the systems are now being used in urology and gynecology as well. They are less invasive than traditional surgery methods and extremely precise, but they cost around $1 million.
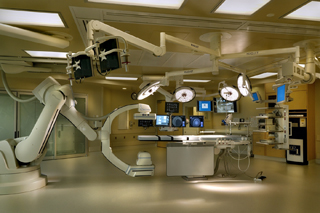
• Interventional. Combining a full surgical suite with imaging devices, ceiling-mounted C-arms are being used for cardiovascular procedures conducted within the surgical suite. Incorporating this imaging equipment into the operating room allows for real-time anatomical imaging viewed on large wall-mounted monitors.
Providence Sacred Heart in Spokane was one of the first 10 hospitals in the United States to employ this hybrid approach, allowing surgeons to combine a traditional case with a minimally invasive one such as an angioplasty.
A multi-axis imaging system known as the Artis Zeego provides continuous 3-D imaging on a combined-use table, avoiding the need to move the patient and adding the ability to angle and tilt the table as needed.
• Interoperational imaging. The least common, incorporating interoperational imaging systems such as mobile MRIs or a CT scanner that allows for high-resolution computer-assisted surgery cases, may represent the future of neurology.
In Tucson, Ariz., St. Joseph’s Hospital is the first facility in the country to install a dual-room intraoperational gantry-mounted CT scanner that slides between two rooms.
Used for complex brain surgery, the CT can be moved into the operating room during the case. Once the imaging is completed, the CT can be slid into a holding area between the operating rooms, making it available to the neighboring room. The shared CT gives the surgical team real-time information about tumors, spinal fusions or vascular malformations before, during and after an operation.
More training space needed
These three high-tech innovations require increased area for equipment and staff, as well as increased sensitivity to floor and structural vibrations that might affect image quality. There is also an increased need to provide training and simulation areas for nurses and surgeons. These expensive tools do not need to leave the surgical suite, so setting aside a simulation room is required.
Hospitals need space to train staff in the use of new technologies and for experienced surgeons to continue to hone their skills. Pressure is mounting from the American Medical Association and federal health officials to expand their continuing education requirements, and even include the entire surgical team in the simulation exercise.
Looking ahead, industry observers see a number of trends that will continue to influence the design and configuration of minimally invasive high-tech operating rooms:
• Continued growth in the use of minimally invasive and noninvasive techniques. Hybrid surgeries will continue to grow, increasing the demand on existing mechanical and electrical systems, increasing space needs and requiring sophisticated data infrastructure and backbone.
• Increased use of robots to leverage their accuracy and reduce recovery times and risk of infection. Much thought has been given to the creation of remote or mobile facilities that take the operating room to the patient.
• Fewer traditional surgeries as advances are made in genetic-based treatments and transplants involving genetically engineered organs.
• Finally, hospitals will continue to struggle with finding the balance between patient desires and budgets. A typical surgical suite can exceed $1 million in construction cost. A surgical robot suite can cost $2 million and a CT almost as much once installed and commissioned. Do hospitals serve potential patient populations large enough to warrant these expenditures? How does an organization balance the desire for the most advanced tools available with the financial realities of the market place?
Erik Goodfriend, AIA, is an associate principal at Mahlum and has over 25 years of architectural experience in the planning, programming and design of health care facilities.
Other Stories:
- Mental health clinic breaking ground in Burien
- Hospitals: get ready for climate change laws
- Federal program keeps money flowing for hospital projects
- MultiCare opens $117M Tacoma campus expansion
- Surgical advances create ‘hybrid’ operating rooms
- In wake of reform, hospitals try doing more with less
- Hospital noise rules get an update