|
Subscribe / Renew |
|
|
Contact Us |
|
| ► Subscribe to our Free Weekly Newsletter | |
| home | Welcome, sign in or click here to subscribe. | login |
Architecture & Engineering
| |
 |
March 4, 2021
The role of ventilation and healthy air
Code Unlimited

Chubb
|
After months of physical distancing and restrictions on public gatherings, people have a renewed appreciation of the value of coming together. Notwithstanding a new appreciation of work-life balance and closeness with our families and significant others, most of us are longing to get back together with others for work, leisure, and learning. Recent work by a Seattle consulting firm has focused on ways to facilitate business openings and operations despite the continuing risk of COVID-19 exposure.
Seattle was among the first metropolitan areas in the U.S. to experience COVID-19, and its effects quickly became clear. Major employers and public officials acted swiftly to curtail the potential for spread by imposing or adopting restrictions on public gatherings and workplace operations. Those who can work remotely have been for months now. Those who could not work from home have been forced to adopt severe limitations on their operations to balance worker safety and health with the need to maintain critical services and facilitate commerce, often at subsistence levels.
Limiting the number of people allowed in shops and restaurants, following physical distancing guidelines, erecting barriers, screening visitors, and mandating mask-wearing are among many precautions workplaces have implemented with varying degrees of success to control exposure and infection. In a few instances, public gathering places have moved their customer service and seating operations outside to take advantage of natural ventilation to limit exposure.
The influence of ventilation on limiting occupants’ exposure to unhealthy conditions is well-established in building regulations and occupational safety and health guidelines. Ventilation requirements focus on limiting the concentrations of hazardous substances, unpleasant odors, temperature and humidity to maintain a comfortable working or living environment.
Other than health care facilities and certain industrial occupancies that produce products for human consumption, heating, ventilation, and air conditioning design practices have not placed much emphasis on understanding or controlling the spread of infectious agents. And the measures mandated in those particular occupancies are not always well-suited to conventional office buildings and other types of workplaces.
At the request of a health care provider, Code Unlimited — a local engineering consultancy — studied the influence of ventilation on the spread of viral droplets from a single cough or sneeze within and beyond an operating room. Using a model known as FaTIMA for Fate and Transport of Indoor Microbiological Aerosols, developed by the National Institute of Standards and Technology, this study helped to understand how conditions in this environment can be applied elsewhere. The findings of these studies suggest we can do more within existing buildings to manage exposures, especially when we understand how droplets and viral particles spread in air within a room or space.
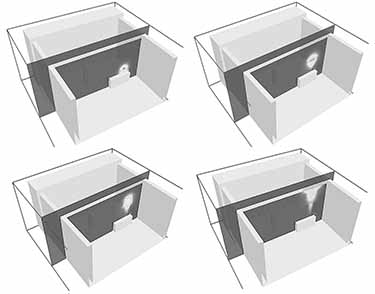
Code Unlimited’s simulation considered a typical 530-square-foot (23 by 23 feet) operating room with 13-foot-high ceilings with an exhaust ventilation rate of 2,800 cubic feet per minute. Viral particles encased in droplets varying in size from 74 to 380 microns remained suspended in the air for just a few minutes until removed by the ventilation system, while some of the larger droplets settled on horizontal surfaces. These simulations suggested that the location and volume of exhaust can make a big difference in reducing human exposures, especially in conjunction with physical distancing, mask-wearing, and other precautions.
To apply these findings to conventional offices and workplace environments, Code Unlimited studied room configurations with lower ventilation rates and different HVAC injection and exhaust points. Most workplace exhaust ventilation rates are about 10% of those in the operating room. Simulations of these environments showed potentially infectious particles remained airborne for much longer periods, sometimes hours rather than minutes.
Air-handling system designs that inject air near the ceiling, exhaust it near the floor, and allow for circulation throughout the space perform much better than systems that inject and exhaust only at the floor or inject near the floor and exhaust near the ceiling. Local filtration systems, such as high-efficiency particulate air (HEPA) filters also mitigate the migration of infectious particles throughout a space.
HVAC designs based on current codes and engineering design principles emphasize comfort and reduce risks that can injure or kill building occupants. Although some of the United States’ earliest building regulations sought to promote hygiene, prevent illness, and improve public health in densely populated urban areas, this emphasis is not so clearly articulated in current code requirements governing HVAC systems when it comes to reducing the transmission of common microbiological agents.
Understanding how HVAC system designs influence the dispersion, condensation, and spread of airborne particles containing infectious agents will help designers, contractors, and building owners create healthier environments for workers and the public. Along with other public health practices these changes can bring us closer to a day when we can gather again with confidence that the risk of infectious disease is manageable.
Mark Chubb is a principal building code and fire analyst at Code Unlimited in Seattle.
Other Stories:
- How to keep the creative spark in a virtual world
- It’s the end of the grocery store (as we know it)
- Are American shopping malls boxed-in?
- Influencing human scale, creating a sense of place
- Here are the 3 principles of renovation
- The future of resilient commercial real estate
- Not all feasibility studies are created equal
- Green Lake Community Center aims for inclusivity
- What if you can’t dig your way out of a brownfield cleanup?
- How A/E firms can increase proposal success in 2021
- Workplace wellness through technology
- 4 Living Buildings: collaborative, courageous, open-minded learning
- Foundations for healthy and sustainable urban places
- Parking garages: rethinking your front door
- A changed workforce and the implications for workplaces and cities